paragraph 1 text
paragraph 2 text
paragraph 3 text

A landmark study in the New England Journal of Medicine reported that minimally invasive vein harvesting for coronary artery bypass surgery was killing patients. Surgical centres across the UK and US abandoned the technique virtually overnight. They returned to traditional open harvesting: a continuous incision from ankle to groin, causing prolonged pain, impaired mobility and high infection rates.
Were the reported harms real? Or had confounding factors distorted the findings?
We provided the definitive answer. Minimally invasive harvesting is safe. It produces better patient outcomes and reduces healthcare costs by more than £2,000 per procedure. Centres resumed the technique. It is now standard care for more than 400,000 coronary bypass operations worldwide each year.

Published studies reported that cardiac MRI induces DNA damage in circulating immune cells. A diagnostic technology used on millions of patients annually might be causing immunological harm. Some researchers called for restrictions analogous to ionising radiation.
Does MRI genuinely cause such damage?
We ran the largest and most comprehensive investigation to date, combining in vitro exposures with in vivo sampling patients undergoing cardiac MRI. We conclusively proved that clinical cardiac MRI does not induce DNA double-strand breaks. It does not compromise immune cell viability or function. We also discovered why the smaller studies got it wrong: the biomarker they relied upon has such pronounced inter-individual variability that underpowered studies were detecting noise, not signal.
The technology is safe. Millions of patients continue to benefit from it.
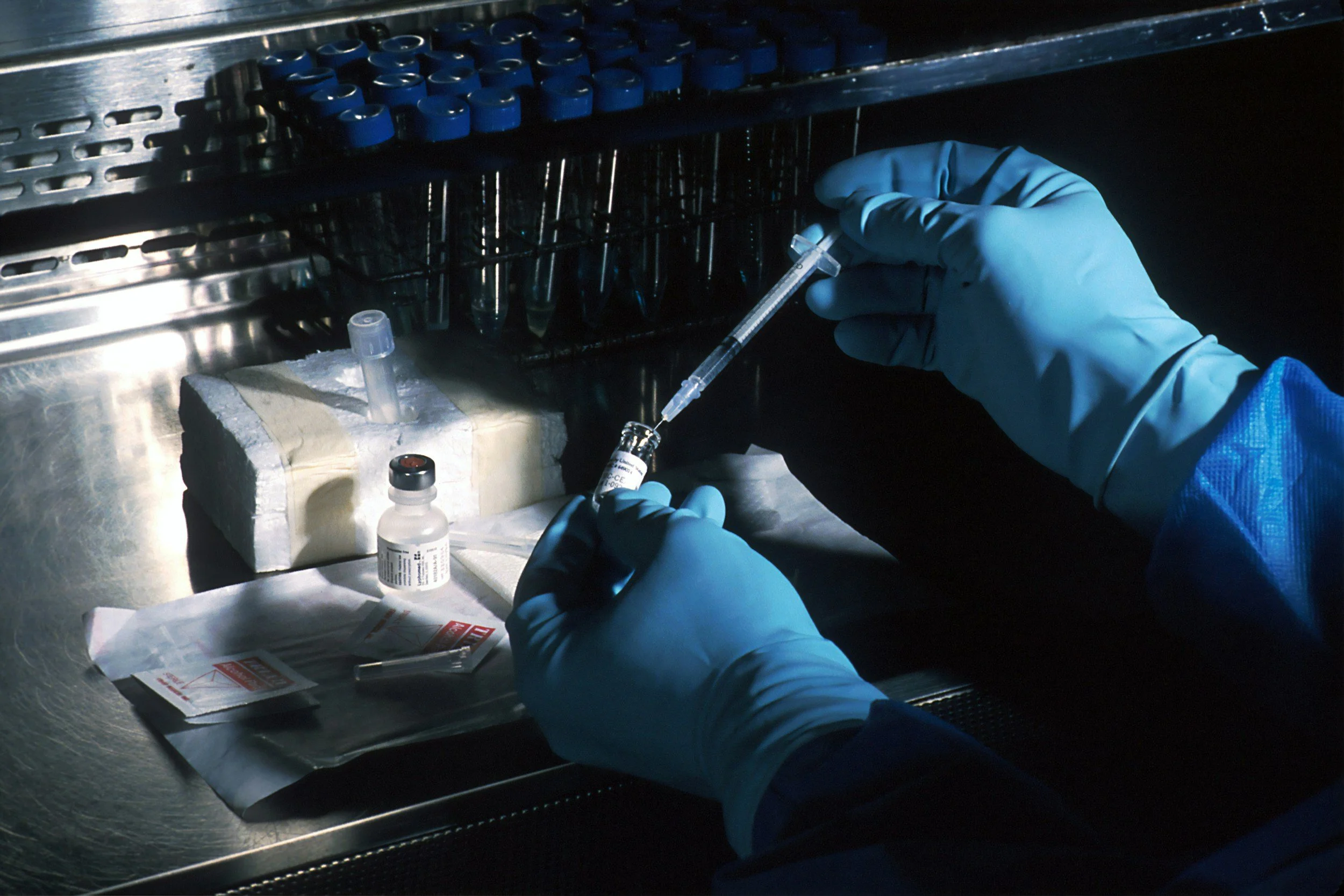
Approximately eighty percent of donated lungs are never transplanted. They are judged unsuitable and discarded, while patients on waiting lists die. Ex vivo lung perfusion, developed by Professor Stig Steen and colleagues at Igelösa, offered a way to evaluate marginal lungs outside the body before deciding whether to transplant.
But could EVLP do more than assess? Could it actively improve the donor lung?
We demonstrated for the first time that it does. EVLP depletes passenger leukocytes from the donor lung, stripping out the inflammatory cells that drive rejection. It upregulates cell survival pathways and downregulates those that induce cell death. The lung that comes out of perfusion is fundamentally better than the lung that went in.
This understanding gave clinicians confidence in the technology. We then performed a multicentre clinical trial, confirming EVLP-reconditioned marginal lungs were comparable to standard transplants. Following FDA approval in 2018 and 2019, organs that would have been discarded are now routinely saving lives.

Hearts undergoing non-ischaemic perfusion were generating immunological responses that would cause severe rejection after transplantation. What was perfusion actually doing to donor hearts?
Using flow cytometry, cytokine profiling, and targeted proteomics, we discovered something unexpected. Perfusion was progressively depleting the heart of its resident leukocyte populations. What looked like an inflammatory storm was actually therapeutic: it was exhausting the donor organ's capacity to attack its future recipient. We confirmed it in transplantation experiments, where immunodepleted hearts exhibited markedly reduced graft infiltration compared with conventional cold storage.
This understanding informed what came next. On 7 January 2022, surgeons at the University of Maryland transplanted a genetically modified pig heart into a fifty-seven-year-old man with terminal cardiac disease using this device.
Transplant patients on immunosuppression need regular blood tests to ensure drug levels are right. Too low and the organ rejects. Too high and the toxicity causes harm. This means frequent trips to outpatient departments, often for years after transplantation.
The clinical team asked us: could we reduce this burden?
We tested how long cyclosporine and tacrolimus remain stable in dried blood spots. Both drugs can be accurately measured from a simple fingerprick sample posted to the laboratory. Patients no longer need to travel for routine monitoring. They take the sample at home, post the card, and the results come back
Fewer hospital visits. Less disruption to patients' lives. The same clinical accuracy.
Post-operative wound complications affect over twenty percent of cardiac surgery patients. Yet the leg incisions required for vein harvesting had received surprisingly little rigorous evaluation. Technologies existed that might help, tissue adhesives and barbed sutures among them, but nobody had tested them in this context.
So we did. In the tissue adhesive study, every patient in the treatment group achieved optimal cosmesis. No patient in the conventional suture group did. Patient satisfaction was substantially higher. We then demonstrated that barbed sutures reduced closure times and healing complications.
These were the first evaluations of these technologies in cardiac surgery. Both are now widely adopted.
Cardiovascular disease is the leading killer of heart and lung transplant recipients. The clinical team asked us: could we improve outcomes without adding yet another pill to patients already burdened with complex medication regimes?
We designed a twelve-month dietary intervention comparing Mediterranean and low-fat diets. Ninety-five percent of patients completed the programme. All of them adhered to their diet. Both intervention groups reduced body mass index, fasting glucose, and total cholesterol. Those who continued with standard diet went in the opposite direction on every measure.
We can identify molecular mechanisms of immunological tolerance. We can also run a dietary study with patients and their families. Problems worth solving exist at every scale.
Kidney preservation by static cold storage is a race against time. Current guidelines permit three to six hours; beyond that, cumulative injury makes organs progressively less viable. In the United States, roughly a quarter of retrieved kidneys are discarded. In the UK, about a hundred kidneys a year are deemed unsuitable after retrieval
Could genuinely physiological perfusion extend safe preservation substantially?
We developed a protocol and tested it head-to-head against the clinical standard. Kidneys on our protocol maintained healthy blood flow, produced urine at normal adult rates, and showed no macroscopic injury. Kidneys on the clinical protocol reperfused poorly, produced grossly abnormal urine volumes indicating tubular injury, and developed multiple infarcts. Every clinical protocol kidney was unsuitable for transplantation. Every one of ours was suitable.
First-in-human transplantation is now planned. If it works: no more emergency overnight surgery, proper time for organ assessment, and more kidneys reaching patients who need them.
Ischaemia-reperfusion injury is paradoxical: restoring blood flow to oxygen-starved tissue causes additional damage through cascading reactive oxygen species. It is a fundamental challenge in transplantation. Biological antioxidants do not help much because they denature and degrade too quickly.
Could synthetic nanoparticles engineered to scavenge reactive oxygen species protect organs during preservation and reperfusion?
Working with poly(propylene sulfide) nanoparticles targeting the reactive species most implicated in reperfusion injury, we demonstrated striking protective effects: more than fivefold reduction in oxidised DNA, substantial drops in inflammatory markers, and stable haemodynamics while untreated organs became acidotic and needed rescue
This is the first therapeutic application of nanomedicine-augmented normothermic machine perfusion. It is proof of concept for an entirely new approach to protecting transplanted organs.
Reconstructive surgeons came to us with a scenario that had no solution. Polytrauma with traumatic amputation: a patient arrives with head and chest injuries and a severed limb. You stabilise the patient first. But while the team saves the life, the limb is dying on a side table. By the time the patient is stable, it is too late
They challenged us to build a system that maintains a limb outside the body long enough for life-saving surgery and reattachment.
We built it. The system now maintains an entire human limb for more than twenty-four hours with no detectable injury.
The technology is moving into another application: transplantation of limbs from deceased donors. A VCA transplant team is now working with our system. First transplant planned for 2026.
A gene therapy company developing AAV vectors for kidney disease had conducted preclinical studies in mice showing no obvious injury. They came to us to evaluate safety before moving toward clinical trials.
The problem was that mice are poor predictors of AAV response in humans. Their kidneys are too small, their vasculature too different, their immune responses not comparable. We designed a delivery protocol that could be replicated clinically: a single pass of the vector across the renal vasculature, followed by 24 hours of perfusion monitoring.
The result was unexpected. The treated kidney developed visible necrosis in the cortex and clot formation in the calyx. The control kidney showed no injury. This was not visible in mice. It would have been visible in patients.
The company now had critical information: their vector causes acute renal injury at this dose via this delivery route. They could adjust dose, modify delivery, or reformulate before reaching the clinic. The protocol we developed for this evaluation has become their clinical delivery protocol
A biotech company had isolated a PKC activator from a tropical plant with potent anti-tumour activity. They wanted to use it for hepatic malignancies, but needed to understand how the liver would respond to direct injection.
We evaluated three doses against vehicle control over 24-hour perfusions in our LIVING-LIVER system. The study revealed something important: the drug's effects remained localised to the injection site, while the vehicle formulation caused diffuse injury throughout all lobes. This distinction, invisible in conventional testing, told them the drug itself was not the problem. The formulation was.
The liver maintained global metabolic function throughout, with complete drug clearance by six hours at lower doses. The company now has safety data to guide reformulation and identify therapeutic windows for clinical development.
A company developing mitochondrial transfer therapy wanted to know whether their approach could improve outcomes for damaged kidneys. Could donated mitochondria enhance recovery after the injury that occurs during organ preservation?
We tested multiple formulations and doses. Kidneys underwent 30 minutes of warm ischaemia and 24 hours of cold storage before 18 hours of reperfusion. One formulation at higher dose showed enhanced blood flow, improved metabolic activity, and better electrolyte balance. Another formulation improved filtration efficiency.
The effects were not universal across all treatments. That was the point. The company learned which formulation works, at what dose, and why. They can now focus development on what the data supports.
A regenerative medicine company developing therapeutic extracellular vesicles needed to know where their EVs go when delivered to a kidney, and whether they cause harm
We perfused kidneys with fluorescently labelled EVs and tracked their distribution. Histological analysis showed EV deposits within glomeruli, inside vessel walls, and in intracellular spaces. Critically, we found no adverse effects: no biochemical derangement, no change in metabolic performance, no difference in haemodynamics between treated and control kidneys
This was the first time the company had seen exactly where their therapy localises in a functioning organ. They also had confirmation of safety across every parameter we measured.
A company developing lipid nanoparticle therapeutics for liver-targeted gene editing needed comprehensive safety evaluation beyond what conventional models could provide.
We ran 30-hour perfusions comparing their LNP formulation against controls, monitoring haemodynamics, metabolic function, liver enzymes, and inflammatory responses across 17 mediators. The extended timeframe allowed us to distinguish immediate treatment effects from delayed responses, and therapy-specific changes from perfusion duration effects.
The company received a complete safety profile: which parameters changed, when, by how much, and whether changes were transient or sustained. Data to support their regulatory submissions and inform clinical development.

